Oct 6, 2021 | Food, Sustainable Development, Wellbeing
By Frank Sperling, Senior Project Manager in the Integrated Biosphere Futures Research Group of the IIASA Biodiversity and Natural Resources Program
Frank Sperling shares his reflections on issues around sustainable and transformational food production in the context of the UN Food Systems Summit.

© Solarseven | Dreamstime.com
Bringing together stakeholders from around the globe, the United Nations Food Systems Summit (UNFSS) calls attention to the opportunities, challenges, and promises that the transformation of our food systems can hold to advance sustainable development.
This transformation needs to happen, while the ongoing Covid-19 pandemic reminds us of the manifold vulnerabilities embedded in our food systems, the inter-dependence of our societies, and the entanglement of human and natural systems. The increases in weather and climate extremes that can clearly be attributed to climate change, ongoing biodiversity loss, environmental degradation, and pollution further illustrate that food systems need to manage a broad range of compounding risks and pressures that play out over different spatial and temporal scales. Advancing and securing gains towards the Sustainable Development Goals (SDGs) will not only require meeting multiple economic, social, and environmental objectives, but also demand pathways that ensure a safe navigation through a treacherous and shifting risk landscape. But how do we build resilience into the food system while transforming it at the same time?
Great strides have been made in technologies and practices that can help food systems manage existing and emerging risks. For example, on the production side, timely access to seasonal forecasts and early warning information coupled with extension services can help farmers to make the right decisions for planting and to anticipate, adapt, and cope with possible shocks. Precision agriculture, which harnesses advances in technology to ensure optimal health and productivity of crops and soils, can reduce the need for inputs. Diversification of livestock and agricultural traits can help farmers to reduce production risks in marginal environmental conditions.
Minimizing the spillover risk of zoonotic diseases, mitigating, and adapting to climatic and environmental changes place additional demands on food systems, but also offer new opportunities. Living sustainably requires comprehensively managing land use, enabling for food production, but maintaining and recovering critical ecosystem goods and services, such as carbon and biodiversity. It requires advancing nature-based solutions, where nature is seen as an ally and not an adversary in delivering on development objectives. Strengthening natural capital accounting and incentivizing environmental stewardship by rewarding actors in the food system for efficient and sustainable management of natural resources, and appropriately informing consumer choices will be important ingredients in reducing the environmental impact as well as environmental vulnerabilities of food systems.
The transformation of the food system is an ongoing process. It is therefore important to understand the impact of different changes across the system. Shifts to healthier diets can have important co-benefits in reducing pressure on the environment and natural resources. Such transformation implies, however, that shifts in demand are also matched by shifts in supply, reflecting appropriate adjustments of agricultural production. To accommodate such system shifts and facilitate system transitions over time, the social resilience and adaptive capacity of society must be addressed accordingly.
Food systems operate at different scales, ranging from local to global. Consequently, the role of trade in ensuring food security and human welfare across a range of contexts is critical. Several countries are already dependent on food imports. Trade can help the food security of regions where agricultural activities become less viable with progressive climate change. At the same time, the changing exposure to socioeconomic and environmental risks arising from the increasing inter-connectivity of societies and economies also need to be addressed, as illustrated by the current pandemic. The evolution of food systems has been largely shaped by a drive for efficiency. We must now consider carefully where efficiency needs to be (counter)balanced with an effort to promote greater diversity, and where we must build in greater redundancy to help manage the variety of risks facing food systems.
Forward-looking approaches aimed at transforming food systems towards greater resilience and sustainability will require a suite of measures within, as well as outside food systems. Such measures entail helping livelihoods and sectors to reduce their vulnerabilities and risk exposure, while also enabling the agility of food systems to manage future risks, avoiding lock-in of structures, which would become mal-adaptive over time. Achieving such transformation will depend on increased collaboration and trust building across sectors, enabling innovation in technologies and practice, strengthening of training and capacity development, and on the improvement of safety nets for reducing vulnerabilities to shocks and managing the social transition. Above and beyond, it requires re-calibrating the connection of food systems with other sectors and systems, such as health, environment, energy, and infrastructure.
The UNFSS in conjunction with the upcoming UN Climate Change Conference in Glasgow (UNFCCC COP26), and the UN Conference on Biological Diversity in Kunming (CBD COP15), are a formidable call to action for political leaders, decision makers in the public and private sectors, scientists, development practitioners, civil society, and to society at large, to come together and jointly imagine and build resilient and sustainable food systems that place people and nature at the center before it is too late.
This blog post was first published on the website of the International Science Council. Read the original article here.
Note: This article gives the views of the author, and not the position of the Nexus blog, nor of the International Institute for Applied Systems Analysis.
Aug 19, 2020 | Climate Change, COVID19, USA, Wellbeing, Young Scientists
By Lisa Thalheimer, 2020 IIASA Young Scientists Summer Program (YSSP) participant in the Risk and Resilience and World Population Programs
Lisa Thalheimer shares her journey in researching climate-related migration in the age of the COVID-19 pandemic and the importance of taking mental health issues into account in climate science and the policy realm.

© Raul Mellado Ortiz | Dreamstime.com
COVID-19 has changed our idea of normal. These unprecedented, stressful times affect us all – some of us more than others. Fear and anxiety over a new disease without any promise of a vaccine anytime soon, global economic downturn, along with feelings of loneliness and emotional exhaustion due to the lockdown, can leave us mentally exhausted. Rates of depression and addiction-related suicide are in fact already on the rise among young people like myself.
Now imagine you are advised to stay at home, but you cannot do so because climate change has turned your entire life upside down: your house is no longer there, you have lost your job, your family or friends – you are likely to feel unhinged. This is a reality for many migrants across the globe. It is inevitable that existing migration patterns will be shifted beyond disasters alone. Cascading impacts form the still unfolding pandemic could compound. No matter if you are a migrant yourself or not, agency and the choice over the decision whether to leave your house or not, and the luxury to socially distance could potentially not be an option with a systemic shock like COVID-19.
These changes in circumstances have also affected me as a young scientist. I would have been in Laxenburg, getting to know my YSSP peers and IIASA colleagues, but this year’s journey has been rewritten – courtesy of the COVID-19 pandemic.
I was living in Oxford in the UK when I came to realise that mental health is a game changer in the way I manage my day, make decisions, my ability to care for my partner who suffers from Amyotrophic Lateral Sclerosis (ALS), and making progress on my PhD thesis. Everything felt more difficult. I was overwhelmed. I wanted to understand why this is the case. My interest soon evolved into researching the links between mental health and my PhD topic of climate-related migration.
For the article “The hidden burden of pandemics, climate change and migration on mental health”, I teamed up with an epidemiologist who specialises in mental health at my old university home, the Earth Institute in New York City. This research experience was an eye-opener, both personally and scientifically.
In our article, we focused on the US, as it has been hit hardest by COVID-19 – in mid-August, the number of COVID-19 cases exceeded five million. On top of this, depression and anxiety are already prominent among Americans, as is costly impacts from disasters. Hurricanes cost the US around US$ 17 billion every year, but estimates show a higher probability of extremely damaging hurricane seasons with climate change. We may know the impact of climate change on assets and on physical health, but what about mental health impacts?

© Raggedstonedesign | Dreamstime.com
Although my coauthor and I come from different scientific disciplines, I soon came to realize that our scientific approach has a common denominator: systems thinking. Accounting for interconnections and cascading effects, our article shed light on different systems affected by COVID-19 and situations where mental health issues are likely to become increasingly prevalent in a changing climate. The article focuses on already vulnerable parts of the population, for example those who have been impacted by Hurricane Katrina or Hurricane Harvey – the latter of which has been made worse by climate change. The article illustrates how COVID-19 becomes a risk multiplier for climate migrants in three distinct case studies: key workers in New York as urban setting, seasonal migration dynamics, and disproportionate effects on black and Latino communities. Unrelenting effects include loss of employment, and a lower likelihood of being able to work from home or to have health insurance than white people.
A better understanding of the mental health-migration-climate change nexus can help absorb adverse mental health outcomes from COVID-19, which would otherwise compound. We however need to tackle systemic risks affecting mental health through synergies in research and policy, and an integrated intervention approach. Free mental health support for key workers through tele-therapy and mental health hotlines provide a practical way forward. Personally, I learned that climate migrants have been relentlessly resilient to systemic shocks. Nevertheless, with mental health issues, it becomes increasingly hard to maintain such resilience. With this commentary, I hope that mental health and interdisciplinary research finds its way in climate science and in the policy realm. We all need a clear mind to attain the Sustainable Development Goals.
Note: This article gives the views of the author, and not the position of the Nexus blog, nor of the International Institute for Applied Systems Analysis.
Mar 10, 2020 | COVID19, Health, IIASA Network, Wellbeing, Women in Science
Raya Muttarak, Deputy Program Director, IIASA World Population Program
Raya Muttarak writes about what we have learnt about the COVID-19 outbreak so far, and how collective mitigation measures could influence the spread of the disease.
© Konstantinos A | Dreamstime.com
Since the outbreak of COVID-19 in Wuhan, China back in January, we have learnt a lot about the virus: we know how to detect the symptoms, and a vaccination is currently being developed. However, there are still many uncertainties:
We for example don’t know enough about the disease’s fatality rate – mainly because we don’t precisely know how many people are infected, which is the denominator. We also don’t know exactly how the virus spreads. Generally, it is assumed that the virus spreads from person-to-person through close contact (within about 1 meter) and through respiratory droplets produced when an infected person coughs or sneezes. It is also thought that COVID-19 can spread from contact with contaminated surfaces or objects.
In addition, knowledge about the timing of infectiousness is still uncertain. There is evidence that the transmission can happen before the onset of symptoms, although it is commonly thought that people are most contagious when they are most symptomatic. This information is crucial, because if we know the timing patterns of the transmission, we could adopt better measures around when to quarantine an infected person.
Lastly, we don’t yet know whether the spread of the disease will slow down once the weather gets warmer.
What is currently happening in Iran, Italy, Japan, and South Korea may be unique to these countries, but it is more than likely that most countries will eventually experience the spread of COVID-19. In this regard, epidemiologists have estimated that in the absence of mitigation measures, in the worst-case scenario, approximately 60% of the population would become infected. In February, Nancy Messonnier, the director of the Centers for Disease Control and Prevention’s National Centre for Immunization and Respiratory Diseases in the US, warned that “It’s not so much of a question of if this will happen anymore, but rather more of a question of exactly when this will happen.”
We learnt from an epidemiological transmission model that public efforts to curb the transmission of the disease should be directed towards flattening the epidemic curve. This is crucial, since the treatment of severe lung failure caused by COVID-19 requires ventilators to help patients breathe in intensive care units (ICUs). Not a single country in the world has the capacity to absorb the large number of people who would need intensive care at the same time. Experience from Italy shows that about 10% of all patients who test positive for COVID-19 require intensive care. Although efforts have been made to increase ICU capacity, the rapidly growing number of infected patients is overloading the healthcare system. Measures to reduce transmission in order to slow down the epidemic over the course of the year will therefore significantly mitigate the impact of COVID-19.
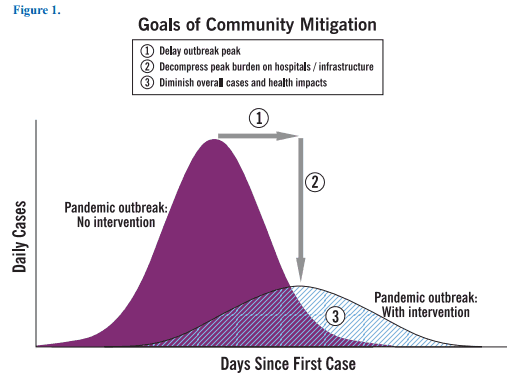
A transmission model with and without intervention.
Source: CDC. (2007). Interim Pre-pandemic Planning Guidance: Community Strategy for Pandemic Influenza Mitigation in the United States—. Centers for Disease Control and Prevention.
The figure above shows the distribution of infectious cases with and without intervention. If the outbreak peak can be delayed, this allows the health system and healthcare professionals to bring the number of persons that require hospitalization and intensive care in line with the nation’s capacity to provide medical care. To flatten the epidemic curve and lower peak morbidity and mortality, calls for both government response and individual actions.
We will have to follow the protocol of the Austrian Health Ministry, but certain practices such as social distancing, washing hands, and avoiding gathering in crowded places, can help reduce the transmission of the disease. While it is true that young and healthy people are less likely to get sick and die from COVID-19, they can still be a virus carrier and thus transmit the disease to other vulnerable subgroups of the population, such as older people and those with underlying health conditions. An article recently published in The Lancet provides helpful information to better understand the current situation and explains why fighting against COVID-19 will take collective action.
Reference:
Anderson R, Heesterbeek H, Klinkenberg D, & Hollingsworth T (2020). How will country-based mitigation measures influence the course of the COVID-19 epidemic? The Lancet 0(0) DOI: 10.1016/S0140-6736(20)30567-5
Note: This article gives the views of the author, and not the position of the Nexus blog, nor of the International Institute for Applied Systems Analysis.
Jan 29, 2020 | Demography, Health, Wellbeing
By Sonja Spitzer, research assistant in the IIASA World Population Program
Sonja Spitzer discusses how survey data often fails to capture all socioeconomic groups and explains how to ensure health information used by policymakers is based on accurate statistics.

Life expectancy continues to increase in Europe. We live longer, but do we live healthier? One way of tackling this question is by analysing health expectancy: a widely used indicator that counts the number of years an average person can expect to live in good health. To create this indicator researchers usually combine information about mortality with health data from surveys – and this is where many problems begin.
Survey participation is shaped by socioeconomic differences
Surveys do not always correctly represent the countries they seek to describe. A common deviation is that highly educated individuals are more likely to participate in surveys than less-educated individuals This is problematic for health research in particular, because highly educated people tend to be healthier than those who are less educated. Overrepresenting healthy and better educated individuals in surveys makes countries appear to have healthier populations than is the actual case. A recent study I conducted, that focused on European countries, showed that health expectancy measures are frequently upward biased, because less-educated people are underrepresented in the underlying data. The results of this study reflect the outcomes of other research; for example, estimates of rates of diabetes and asthma in Belgium are too low because individuals with a high level of education are overrepresented in the core data. In the Netherlands, the underrepresentation of those with lower levels of education has led to underestimating smoking prevalence, alcohol intake, and low levels of physical activity.
Make everyone count with statistical weights
Are you now wondering if you can ever trust health measures again? Do not despair! Surveys can still be a very useful source for answering health-related questions if the appropriate statistical tools are used. It is possible to account for the misrepresentation of participants with lower levels of education in surveys. The only thing needed is accurate information about the education structure of the population, that is: How many highly educated versus less-educated individuals live in a given country? In Europe, this information is readily available via censuses. Using information from censuses makes it possible to calculate statistical weights for surveys. If the less educated are underrepresented in surveys, each observation of a less educated individual is weighted relatively more than those with a higher level of education to account for the misrepresentation. This weighting enables surveys to resemble the population in the real world and the health measures that are based on them to no longer be biased by educational differences in survey participation.
Why do the less educated not participate in surveys?
Using survey methods such as statistical weights might become even more necessary in the future – it appears that the gap in survey participation between the higher and the less-educated is increasing year upon year. Those with low levels of education are frequently more difficult to engage, for example, less educated people can have less stable life paths and thus more often change their address. They may be less likely to provide requested information in surveys because they are too sick to participate or are less aware of the details of their health and financial situation. Finally, survey participation is usually voluntary and those with lower levels of education are more likely to refuse participation. One could speculate that this refusal to participate is because we, as researchers fail to engage with, or reach out to, less-educated individuals and the “value” of participating in surveys is therefore not well-communicated. This concern seems particularly important in the age of ‘fake news’. If less-educated individuals were better represented in surveys, this would make official statistics more reliable and might also lead to a better appreciation of statistics and how they can be more profound indicators than, for example, an opinion posed by someone on TV.
References:
[1] Demarest, S., Van Der Heyden, J., Charafeddine, R., Tafforeau, J., Van Oyen, H., Van Hal, G.: Socio economic differences in participation of households in a Belgian national health survey. European Journal of Public Health. 23, 981–985 (2013). DOI:10.1093/eurpub/cks158
[2] Korkeila, K., Suominen, S., Ahvenainen, J., Ojanlatva, A., Helenius, H.: Non-response and related factors in a nation-wide health survey. European Journal of Epidemiology 17, 991–999 (2001)
[3] Reinikainen, J., Tolonen, H., Borodulin, K., Härkänen, T., Jousilahti, P., Karvanen, J., Koskinen, S., Kuulasmaa, K., Männistö, S., Rissanen, H., Vartiainen, E.: Participation rates by educational levels have diverged during 25 years in Finnish health examination surveys. European Journal of Public Health. 28, 237–243 (2018). DOI:10.1093/eurpub/ckx151
[4] Spitzer, S., Biases in health expectancies due to educational differences in survey participation of older Europeans: It’s worth weighting for. The European Journal of Health Economics. (2020) IIASA doi:10.1007/s10198-019-01152-0. http://pure.iiasa.ac.at/id/eprint/16281/
Note: This article gives the views of the author, and not the position of the Nexus blog, nor of the International Institute for Applied Systems Analysis.
Oct 31, 2017 | Health, Wellbeing
By Anastasia Aldelina Lijadi, research scholar in the IIASA World Population Program
What does happiness mean? The concept of “happiness” has somewhat abstruse meanings in different languages. Some suggest the idea of luck or good fortune (German, Norwegian, French, Korean, Russian, Japanese, Chinese) and others intimate satisfaction of one’s desires or wishes and goals and enjoyable experiences (Italian, Portuguese, Spanish). Anthropologists, economists, linguists, psychologists, sociologists, and other researchers from various disciplines are still struggling to operationalize the concept, and ensure that enhanced quality of life is a realistic and obtainable goal for human kind.
As part of the project Empowered Life Years, at the World Population Program at IIASA, the concept of happiness has been identified as one of the conditions for sustainable human wellbeing, along with health, literacy, and being out of poverty. Being the newest in the team, I was privileged to attend the 15th annual conference of International Society for Quality-of-Life Studies (ISQOLs) to attend lectures and presentations and better comprehend the concept of happiness and how this research-based knowledge can contribute to people’s wellbeing.
Six supports for happiness
The distinguished keynote speaker Prof. John F. Helliwell specified six prerequisites for a human being to be happy, which are material (such as food and shelter), relationships, mental and physical health, freedom from oppression, generosity, and trust. His studies showed that mental and physical health is more effective in increasing happiness than raising income or ending unemployment. Moreover, people are more generous (i.e., show strong altruism or pro-social behavior such as donating blood, or care for environment) when they have a good social relationships within their community.

Keynote lecture at the ISQOLs conference. © Anastasia Aldelina Lijadi | IIASA
Measuring Happiness beyond GDP: How and for whom?
It is hard to tell what does cause (un)happiness in a country when wealth has failed to fully explain it. The Easterlin Paradox claims that a society’s economic development and its average level of happiness are not linked beyond a certain level of income that satisfies basic needs. This is the case in Latin America, as Prof. Mariano Rojas, president of ISQOLs, pointed out in his presentation. Bhutan also fits this theory, said Prof. Shrotyia Vikar Kumar of the University of Delhi, as it has controversially the highest happiness index in the world despite low GDP.
In addressing income inequality, Prof. Richard Wilkinson of the London School of Economics, stressed that the story is the same in unequal societies worldwide: men in poorer households feel low, outcast, and very sensitive to what others think about them, wives loathe their husbands, and children ashamed of their condition. We witness a higher discrepancy in health, crime, infant mortality, and civic participation between rich and poor communities. The rich also rate themselves better than poorer people, and are more likely to search for ‘status goods’ in google!
Prof. Antonella Delle-Fave, University of Milan, urged us to review the construct of happiness before trying to measure it. She also criticized the polarizing and overused concepts of hedonic and eudemonic happiness. Hedonic happiness is based on the experience of pleasure or positive feelings while generally avoiding any painful experiences. Eudemonic happiness is the notion of wellbeing based on the pursuit of personal fulfillment and realizing one’s potential by engaging in meaningful activity. Delle-Fave found that many researchers use a mix of variables derived from both concepts.
Prof. Richard Layard, author of Happiness: Lessons from a New Science, stated that happiness evolves over the life course. A simple cross-sectional correlation study cannot explain the evolution of happiness throughout life course, and Layard urged future research to employ an interdisciplinary approach to find the determinants of happiness. This will help policymakers to create meaningful, accessible, and age-sensitive opportunities for promoting quality of life throughout a lifetime.
Prof. Delle-Fave added that bottom-up qualitative research is needed to define happiness, eliciting voices directly from the source: “After learning from university, we need to learn from people.” I will use this powerful yet simple advice in my work on Empowered Life Years at IIASA.
Note: This article gives the views of the author and not the position of the Nexus blog, nor of the International Institute for Applied Systems Analysis.








You must be logged in to post a comment.